How to Calm a Lipedema Flare-Up Fast
- Ella
- Mar 7
- 4 min read
Updated: 1 day ago
A lipedema flare up can feel like it comes out of nowhere.
One day your symptoms feel manageable.
The next, everything hurts more. Swelling increases.
Your legs feel heavier, tighter, and more painful. Clothing fits differently. Even walking feels harder than usual.
If you’ve been through this, you already know the worst part: once a flare starts, it can spiral quickly if you don’t intervene.
The good news? A flare is not random — and it’s not unstoppable.
Lipedema flares follow very predictable physiological patterns, which means there are specific things you can do immediately to calm your system and shorten the duration of the flare.
Below are the five most effective steps to take right now when a lipedema flare begins.
What Actually Triggers a Lipedema Flare Up?
Before we get into the steps, it helps to understand what’s happening inside your body.
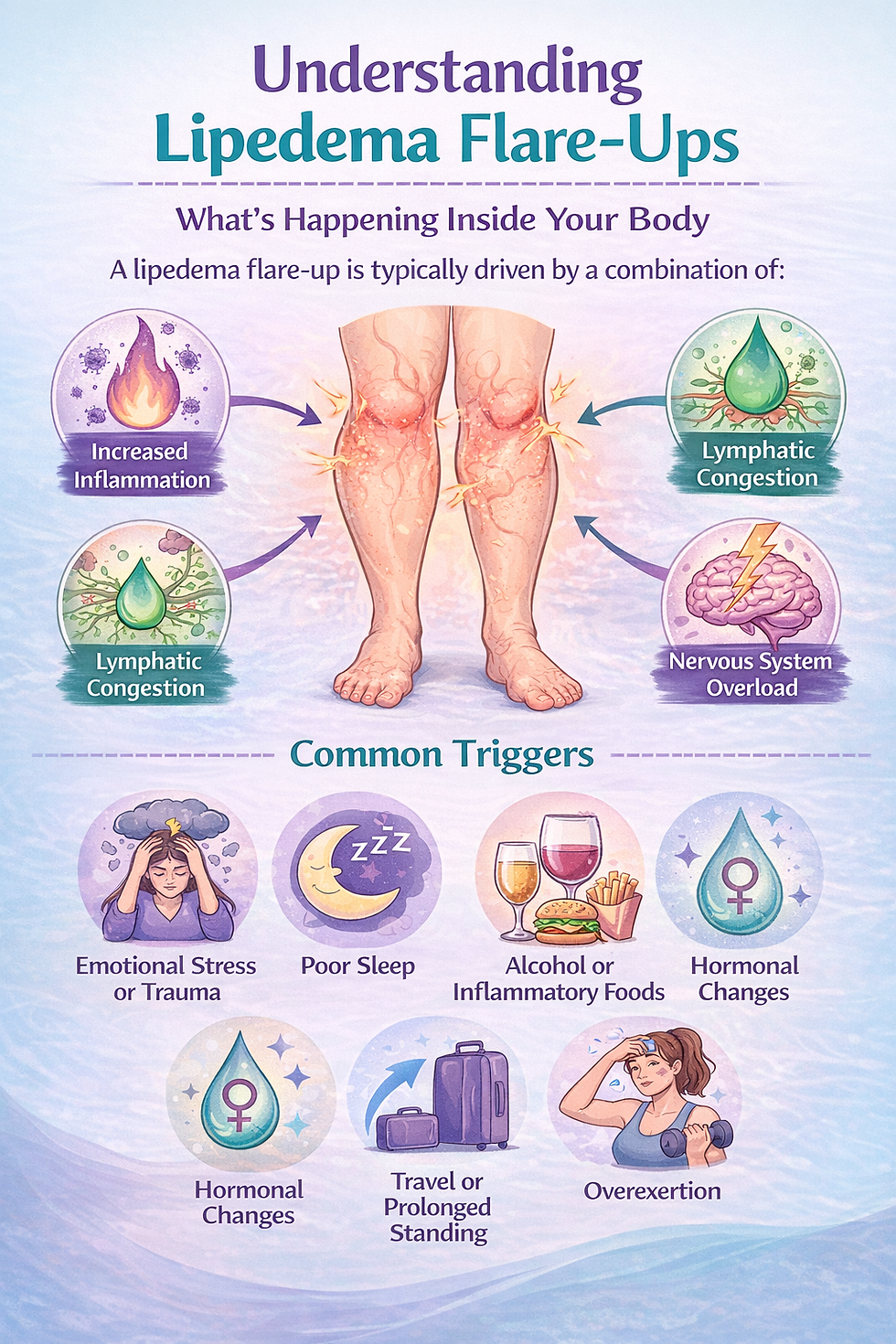
A lipedema flare up is typically driven by a combination of:
Increased inflammation
Lymphatic congestion
Nervous system overload
Hormonal or metabolic stress
Pain researchers have shown that lipedema involves altered pain signaling and heightened inflammatory responses, meaning once your system is triggered, symptoms can amplify rapidly if the underlying drivers aren’t addressed, as discussed in clinical pain research.
That’s why flares often follow:
Emotional stress or trauma
Poor sleep
Alcohol or inflammatory foods
Hormonal changes
Travel or prolonged standing
Overexertion
A flare isn’t failure. It’s a signal.
And signals can be responded to.
Step 1: Get on a supplement immediately (this works around the clock)
When a lipedema flare up hits, your body needs constant support, not something you do once a day and forget.

This is where supplements matter most.
A targeted supplement helps address flare drivers 24 hours a day, supporting:
Lymphatic flow
Microcirculation
Capillary stability
Inflammatory signaling
Unlike diet or exercise, supplements don’t require energy, motivation, or discipline during a flare — when you’re already depleted.

That’s why many women rely on a comprehensive option like Lipera during flares.
It supports the systems involved in pain, swelling, and heaviness continuously, even while you’re resting or sleeping.
During a flare, consistency matters more than perfection.
This step is foundational.
Step 2: Immediately lower stress (this is not optional)
Stress is not a side issue — it is a primary flare accelerant.
During a lipedema flare up, the nervous system is already overstimulated. Cortisol rises.
Lymphatic flow slows. Inflammatory signaling increases. Pain sensitivity goes up.
If stress stays high, the flare lasts longer. Period.
That’s why your next move should be something that visibly and measurably calms your system, even if only for a short time.
Examples that actually help:
A massage (even a short one)
A warm bath with bath salts or oils
A quiet meditation class
Gentle breathwork
Lying down in a dark, calm space
The goal is not luxury. It’s nervous system regulation.
Research shows that inflammatory pain conditions worsen under sustained stress, reinforcing why calming interventions are essential during flares, as explored in neuroinflammation research.
Think of stress relief as treatment — not self-indulgence.
Step 3: Elevate your legs as much as possible

Elevation is one of the fastest ways to reduce fluid congestion during a lipedema flare up.
When you elevate your legs:
Lymphatic drainage improves
Venous pressure decreases
Tissue tension softens
This doesn’t need to be extreme. The key is frequency and duration.
Try:
Elevating legs above heart level several times per day
Sleeping with legs slightly elevated
Taking breaks from sitting or standing
Even modest elevation can help interrupt the fluid buildup that fuels swelling and pain during flares.
This step is simple — but extremely effective when done consistently during the acute phase.
Step 4: Cut out inflammatory foods and alcohol immediately
Food choices matter most during a flare — not because diet caused it, but because inflammation determines how long it lasts.
During a lipedema flare up, your body is already inflamed. Adding inflammatory inputs only prolongs the reaction.
This means:
No alcohol
No ultra-processed foods
No sugar spikes
No inflammatory oils
Alcohol is a particularly strong trigger because it:
Increases inflammation
Disrupts lymphatic flow
Worsens fluid retention
Many women notice dramatic flare worsening when alcohol is present, which is why it’s consistently listed among flare triggers, as outlined in this lipedema trigger breakdown.
During a flare, the goal isn’t dietary perfection — it’s damage control. Simple, anti-inflammatory meals can noticeably shorten flare duration.
Step 5: Compression + gentle movement (not intense exercise)
Compression and movement work best together — especially during a flare.
Compression
Compression helps by:
Supporting lymphatic return
Reducing tissue expansion
Limiting fluid accumulation
During a lipedema flare up, consistent compression can reduce heaviness and pain significantly.
This is one of the most underused tools during acute flares.
Gentle movement
Movement should be gentle and rhythmic, not exhausting.
Helpful options include:
Short walks
Light cycling
Easy mobility work
The goal is to activate the muscle pump without triggering additional inflammation.
High-intensity workouts during a flare often backfire.
Gentle movement supports lymphatic flow without stressing the system.
If leg discomfort is a major issue, movement strategies can help you stay active without worsening symptoms.
What to Expect After You Intervene

When these steps are applied early, most women notice:
Reduced pain intensity
Less swelling progression
Shorter flare duration
Faster return to baseline
What prolongs flares most often:
Ignoring early symptoms
Pushing through stress
Drinking alcohol “just once”
Overexertion
Skipping compression
A lipedema flare up is much easier to calm in the first few days than after weeks of compounding inflammation.
Conclusion on Flare Ups
A lipedema flare up is not something you have to endure passively.
It’s a physiological response — and physiological responses can be interrupted.
The most effective strategy is layered:
Support your system continuously with supplementation
Calm your nervous system immediately
Reduce fluid congestion through elevation
Remove inflammatory inputs
Use compression and gentle movement to keep fluid moving
The faster you respond, the shorter the flare.
And over time, consistently managing flares this way often leads to fewer flares overall — because your body learns that it is supported, not overwhelmed.



Comments